In addition, they can cause hypertension and cardiovascular disease.
Today’s blog post looks at how OSA can be improved in order to lead to better prognoses for patients as well as an increase in their quality of life. IMT, for example, was tested to see if it can cause an improvement of OSA in patients with mild to moderate forms of the disorder. Let’s take a closer look at the study below.
Key Findings
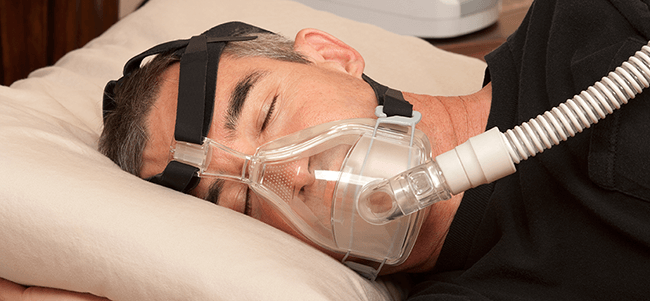
- Obstructive sleep apnea (OSA) is characterized by reduced or stopped airflow, leading to awakening, reductions in blood oxygen levels and disturbed sleep architecture.
- OSA leads to impaired daytime activities, cognitive function, work performance, quality of life (QOL) and can cause hypertension and cardiovascular disease.
- 6 weeks of respiratory muscle training (RMT) reduced awakenings, arousals, and limb movements.
Patient Impact
RMT effectively improves sleep quantity and quality in people with OSA.
Study Methods
A wide variety of variables were addressed throughout the course of this study, including:
- Sleep (duration, quality, architecture, and apnea hypopnea index)
- Blood pressure (systolic and diastolic pressures)
- Plasma catecholamine content (epinephrine, norepinephrine, and dopamine)
- T lymphocyte populations (pro-inflammatory Th1, Th2, and Th17 helper T cells, cytotoxic T cells, and anti-inflammatory regulatory T cells)
All of the above were assessed in patients with mild to moderate OSA before and after six weeks of daily IMT. IMT included 30 breaths per day at 75% PImax for six weeks. Results were compared to a low intensity control group.
Study Results
IMT resulted in significant reduction of awakening after sleep onset, reduction in arousal per hour or sleep and limb movement, and improvement of sleep quality. Furthermore, IMT lead to increased PImax and significantly lower blood pressure.
Respiratory muscle training using IMT significantly improves sleep quantity and quality in persons with OSA, reduces apnea and lowers blood pressure.
Does having a thornwalt cyst also may also halt breathing at night and/or awakening at night or making to the morning trying to breathe be a factor why this disease persists. I do have sleep equipment.
Hi Sandra,
Thank you so much for reaching out to us regarding your concern. I am more than happy to assist you with this matter!
RMT has proven beneficial in some studies in patients with CF. Especially in combination with exercise, RMT may increase your respiratory muscle strength, exercise tolerance, and oxygen uptake. In addition, RMT may reduce the frequency of exacerbations. You can ask your physician if the thornwaldt cyst would be an issue for RMT as it is completed with the Breather via mouthpiece. This only requires a small palate to increase a seal by closing off your nasal passage at the nasopharynx. Additionally, it seems like you have a case of sleep apnea, which is likely the culprit of apnea events & awakenings during the nights. In this case I would also recommend you reach out to your health care provider regarding this matter. If you wish to see the benefits of RMT with the Breather and sleep apnea please see this helpful link attached: https://www.pnmedical.com/therapeutic-use/other-diseases/effect-of-rmt-on-sleep-architecture-in-obstructive-sleep-apnea/
If you have any further questions, please do not hesitate to contact us.
Kindest regards,
Quamarul Manna
PN Medical
In this article, we’ll look at how Respiratory Muscle Training (RMT) can help people who suffer from obstructive sleep apnea. A better night’s slumber may be the result of the author’s explanation of how RMT can increase the strength and endurance of respiratory muscles. In addition to discussing the benefits of RMT for treating sleep apnea, the article includes study results proving its efficacy. This article is a great resource for anyone thinking about trying RMT therapy or researching alternative sleep apnea treatments.