Arnold RJ and Bausek N. Effect of respiratory muscle training on dysphagia in stroke patients—A retrospective pilot study. Laryngoscope Investig Otolaryngol 2020, 1-6.
NOTEWORTHY ATTRIBUTES OF THIS STUDY
- In contrast to most clinical studies, which focus on strengthening expiratory muscles, this study uses cRMT (combined Respiratory Muscle Training), simultaneously strengthening the inspiratory and the expiratory muscles.
- This study assesses both objective clinical outcomes for swallowing, as well as patient perception, which is an important aspect of health-related quality of life.
- This study shows that 28 days of using THE BREATHER significantly improves swallowing function as well as patient perception of their swallowing.
- This study shows for the first time that four weeks of cRMT using THE BREATHER improves swallowing function and airway protection. These improvements can help people with dysphagia to reduce the risk of malnutrition, social isolation, morbidity and mortality, and can greatly improve the quality of life.
- Dysphagia post stroke is still underrecognized and undertreated in a number of healthcare facilities.
SUMMARY OF KEY RESULTS
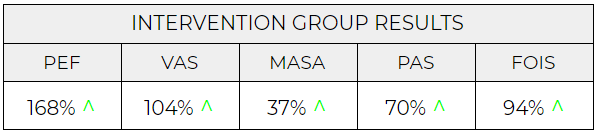
PEF: peak expiratory flow, VAS: visual analog scale, MASA: Mann Assessment of Swallowing Ability, PAS: Penetration Aspiration Scale, FOIS: Functional Oral Intake Scale.
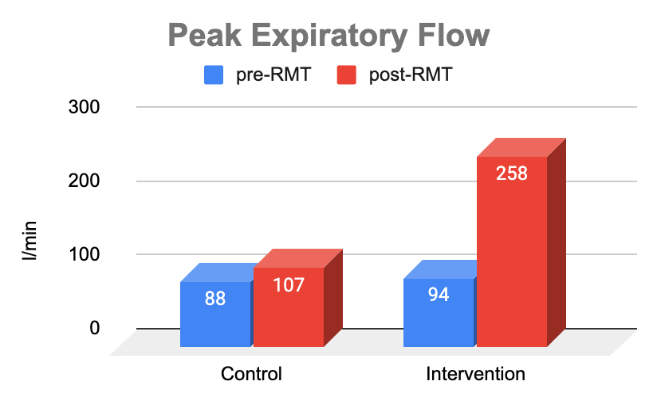
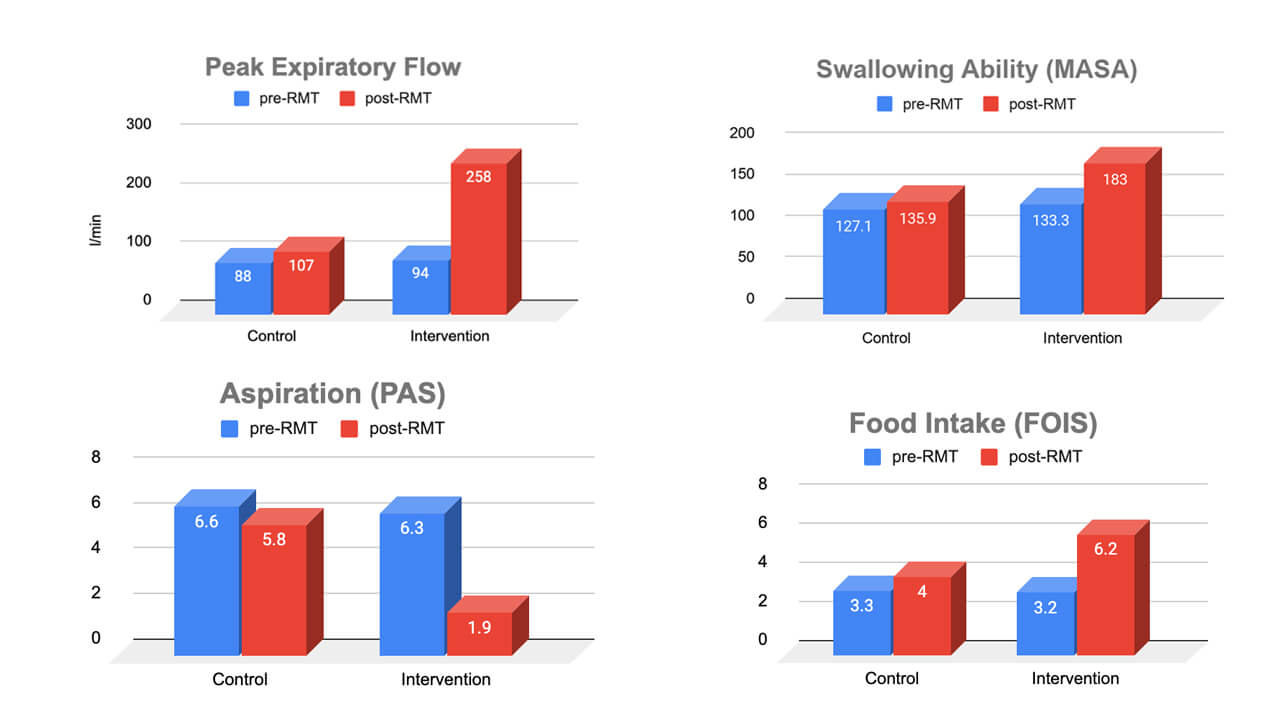
- This study shows that using THE BREATHER for 4 weeks improves airway protection by 168% in people with dysphagia following stroke (measured by PEF)
- This study shows that using cRMT with THE BREATHER improves the perception of swallowing dysfunction by 104% within 28 days in people with dysphagia post stroke
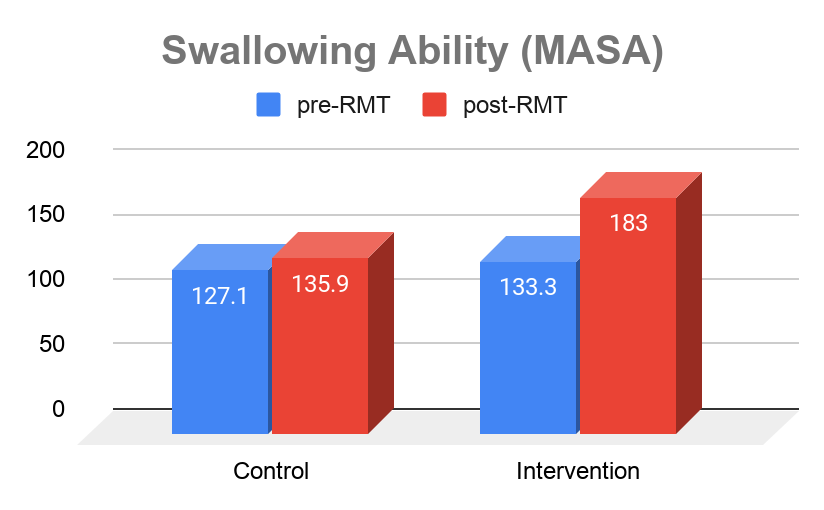
- Using THE BREATHER improve clinical outcomes of swallowing function (assessed by MASA) by 37% within 28 days in people with dysphagia after stroke
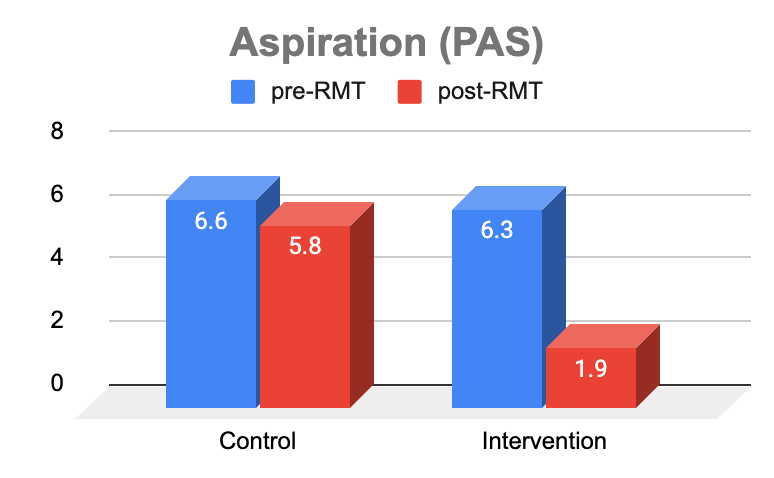
- Aspiration of food and liquid can cause pneumonia and contributes to mortality after stroke. Four weeks of using THE BREATHER reduces aspiration by 70% in people with dysphagia after stroke
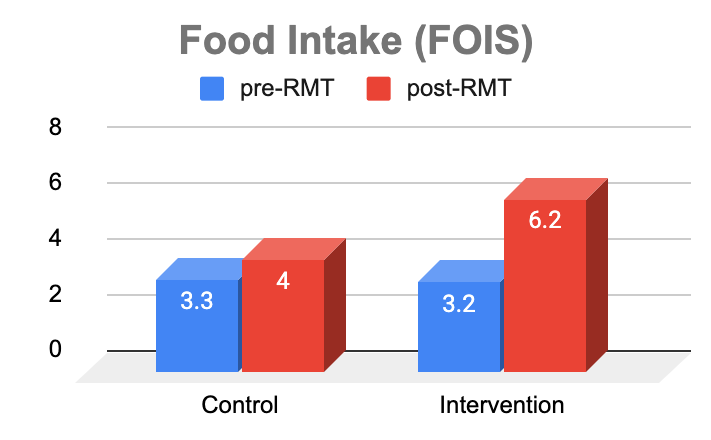
- Dysphagia following stroke can lead to malnutrition, social isolation, and reduced quality of life. Four weeks of using the Breather improved the ability to eat and drink a range of consistencies again by 94%
BRIEF
Swallowing is a complex multi-phase neuromuscular sequence that is generally completed without a thought in the general population. While the intake of food and liquid is the more obvious role of the swallowing reflex, another important role is airway protection. Coordination of respiration and swallow is critically important as both take place within the laryngeal complex, but cannot safely occur simultaneously. When food or liquid gets aspirated, it enters the airways, and can lead to airway infections including pneumonia. Dysfunctional swallowing, or dysphagia, causes 60,000 deaths every year in the US, mainly due to complications of aspiration pneumonia. Dysphagia mainly affects the elderly over 65 years of age, and is particularly prevalent after stroke. People who suffer from dysphagia after stroke are more likely to die within 90 days than those who have normal swallow function. Despite these figures, dysphagia remains underrecognized and undertreated in many healthcare settings.
As breathing and swallowing are interconnected, both processes require activation and control of the respiratory muscles. Strengthening of the respiratory muscles by respiratory muscle training (RMT) has therefore been considered a feasible approach to improve swallow dysfunction. The Breather is the first RMT device invented forty years ago by respiratory therapist Peggy Nicholson, and has been used by a growing number of patients and clinicians ever since. In contrast to many of the commonly used RMT devices, the Breather strengthens both inspiration and expiration by providing resistance, and training intensities can be adjusted independently for each muscle group. This combined RMT (cRMT) therefore strengthens all respiratory muscles required for effective and safe swallowing. Researchers have now looked at and analyzed original data on the effectiveness of using the Breather in patients with dysphagia after stroke.
Data collected in cooperation with a pro bono medical service included patients presenting with dysphagia post CVA. Patients were provided a choice of being trained using the Breather during wait times for traditional therapy services. The data of ten patients who chose to use the Breather was compared against a control group of ten patients who chose not to do RMT. After 28 days of using the Breather, or, in the case of the control group, of not doing any therapy, the baseline measurements were repeated and compared.
OUTCOMES
This study looked at the swallowing ability and the swallowing safety of the patients, as well as of the subjective experience of swallowing. The main results table of the retrospective study “Effect of respiratory muscle training on dysphagia in stroke patients—A retrospective pilot study” by Dr Bob J. Arnold shows that all five individual assessments improved significantly in those patients who used the Breather for four weeks, while it did not change in the control group. Patients who used the Breather were able to safely take in a wider range of food consistencies again, and had a more effective cough function, improving their airway safety and reducing the risk of aspiration.
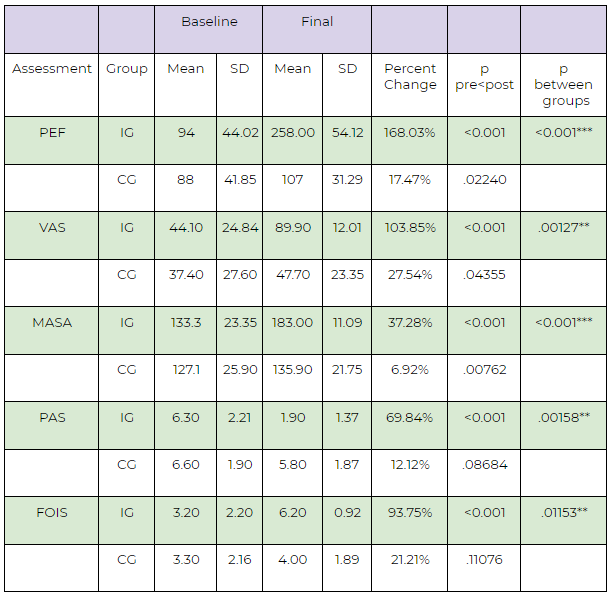
TABLE OF RESULTS
Baseline data and data collected at the end of the 4 week intervention. Abbreviations: IG: intervention group, CG: control group, SD: standard deviation, p: p-Value (T-Test, two tailed), PEF: peak expiratory flow, VAS: visual analog scale, MASA: Mann Assessment of Swallowing Ability, PAS: Penetration Aspiration Scale, FOIS: Functional Oral Intake Scale. Asterisks (*) indicate level of statistical significance.
0 Comments