Science Blog

The Role of Cardiopulmonary Fitness in Weight Loss
Key Findings: Obesity reduces cardiorespiratory fitness (CRF), leading to decreased lung capacity and increased oxygen demands during physical activities, resulting in fatigue and exertional dyspnea. Improved CRF is associated with positive changes in body composition...

The Burden of Dementia: A Global Challenge
Key Findings As of 2019, more than 55 million people have dementia worldwide, over 60% of whom live in low-and middle-income countries. Every year, there are nearly 10 million new cases. The global economic burden of dementia is over $1.3 trillion per year Chronic...

How RMT can reduce blood pressure and the risk of cardiovascular disease
Key Findings Respiratory Muscle Training (RMT) improves inspiratory muscle strength, lowers blood pressure, and improves endothelial function and circulation RMT reduces inflammation and increases cardiovascular health biomarkers The benefits of RMT persist even after...

The Power of Breathing: Enhancing Voice Production and Performance through Respiratory Muscle Training
Context and Key Findings Speech and singing rely on controlled airflow, subglottic pressure, and appropriate lung volume. Respiratory muscles, including the diaphragm, play a critical role in voice production. Singers can optimize voice quality through well-developed...

Meta-Analyses: Improvement in Blood Pressure, Pulmonary Functions, and Sleep Quality by IMT in OSA patients
By Noman Elahi, M.Phil.CLINICAL CONTEXT AND KEY FINDINGS The cessation of sleep due to complete or partial obstruction of upper air passages is the characteristic symptom of obstructive sleep apnea (OSA) Hypertension has been reported in more than 50% of the OSA...
Should RMT be recommended for patients at risk of prolonged hospitalization?
Blog article; Jan 8, 2018 Should respiratory muscle training (RMT) be recommended for patients at risk of prolonged hospitalization? Respiratory muscle training (RMT) has proven effective in the pre- and postoperative care to prevent respiratory muscle weakness....

Improve the quality of your voice with RMT
Speech is produced by moving air against the resistance in the larynx or throat through the narrowed glottis and vocal folds. Speech production depends on appropriate lung volume and subsequent chest wall pressure created by this volume. At higher lung volumes, the...
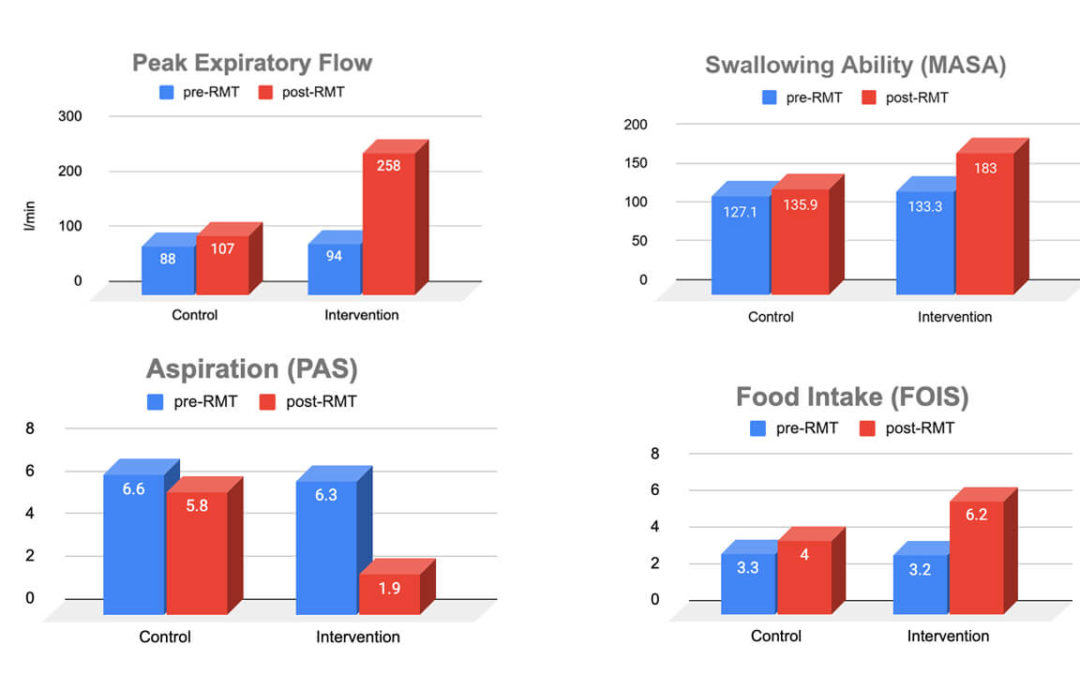
EFFECT OF RESPIRATORY MUSCLE TRAINING ON DYSPHAGIA IN STROKE PATIENTS—A RETROSPECTIVE PILOT STUDY
Arnold RJ and Bausek N. Effect of respiratory muscle training on dysphagia in stroke patients—A retrospective pilot study. Laryngoscope Investig Otolaryngol 2020, 1-6. NOTEWORTHY ATTRIBUTES OF THIS STUDY In contrast to most clinical studies, which focus on...

FLU, PNEUMONIA & COVID-19 UTILIZING RESPIRATORY MUSCLE TRAINING FOR RISK-REDUCTION, TREATMENT & RECOVERY
Respiratory muscles are not only critical elements for breathing, they also function as key components of the speech and swallow mechanisms, even support your posture, balance, and core strength. What if respiratory muscles could also help to reduce the risk of...
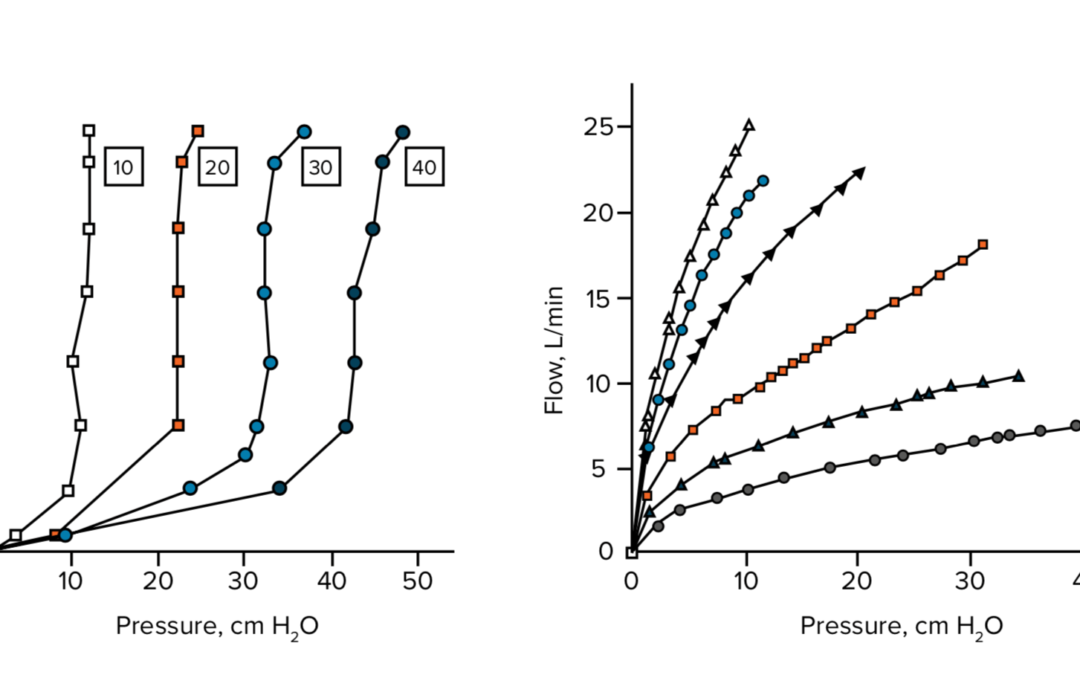
HEAD TO HEAD: THE BREATHER VS THRESHOLD RMT DEVICES
Respiratory Muscle Training using a resistive load device improves quality of life in patients with COPD more effectively than threshold load devicesRespiratory muscle training (RMT) can be applied for training, treatment, preven- tion or rehabilitation in a wide...
Search All Articles